The male reproductive system performs several interconnected functions: producing sperm cells, synthesising the male sex hormone testosterone, and delivering sperm during reproduction. Each structure, from the testes to the vas deferens, plays a specific role. Understanding the primary function of male reproductive system structures provides necessary context for understanding fertility, hormonal health, and common male health conditions.
The male reproductive system functions to produce sperm (spermatogenesis), secrete testosterone, and transport and deliver sperm for fertilisation. These functions are coordinated through a hormonal feedback loop between the hypothalamus, pituitary gland, and testes.
Key Structures and Their Functions
| Structure | Primary Function |
|---|---|
| Testes | Sperm production (spermatogenesis) + testosterone synthesis |
| Epididymis | Sperm maturation and storage |
| Vas deferens | Sperm transport from epididymis to urethra |
| Seminal vesicles | Produce fructose-rich fluid (60% of semen volume) |
| Prostate gland | Produces alkaline fluid that protects sperm; adds to semen volume |
| Bulbourethral (Cowper’s) glands | Produce pre-ejaculatory fluid that neutralises urethral acidity |
| Urethra | Common pathway for urine and semen (not simultaneously) |
| Penis | Delivers semen during intercourse; urine during urination |
Testicular Function in Detail
The testes perform two distinct but related roles:
Spermatogenesis (Sperm Production)
- Occurs in the seminiferous tubules within the testes
- Requires temperature 2-3°C below core body temperature – which is why the testes are external
- Takes approximately 70-74 days from germ cell to mature sperm
- A healthy adult male produces approximately 1,500 sperm per second
- FSH (follicle-stimulating hormone) from the pituitary stimulates spermatogenesis
Testosterone Production
- Produced by Leydig cells in the testes
- LH (luteinising hormone) from the pituitary stimulates Leydig cell testosterone secretion
- Testosterone drives: secondary sexual characteristics, muscle mass, bone density, libido, mood, red blood cell production, and spermatogenesis itself
The Hormonal Axis
The male reproductive hormonal system (HPG axis):
- Hypothalamus releases GnRH (gonadotropin-releasing hormone)
- Pituitary gland responds by releasing LH and FSH
- LH → stimulates Leydig cells → testosterone production
- FSH → stimulates Sertoli cells → supports spermatogenesis
- Negative feedback – testosterone and inhibin B feed back to suppress GnRH, LH, and FSH, maintaining balance
Semen Composition
Semen is not just sperm – it’s a complex fluid designed to support sperm survival:
| Component | Source | Function |
|---|---|---|
| Sperm | Testes | Carries genetic material |
| Fructose-rich fluid | Seminal vesicles (60%) | Energy source for sperm motility |
| Alkaline fluid | Prostate gland (30%) | Neutralises vaginal acidity; liquefies semen |
| Pre-ejaculatory fluid | Bulbourethral glands (5%) | Neutralises urethral acidity; lubrication |
| Other secretions | Epididymis | Sperm maturation support |
Sperm Journey to Fertilisation
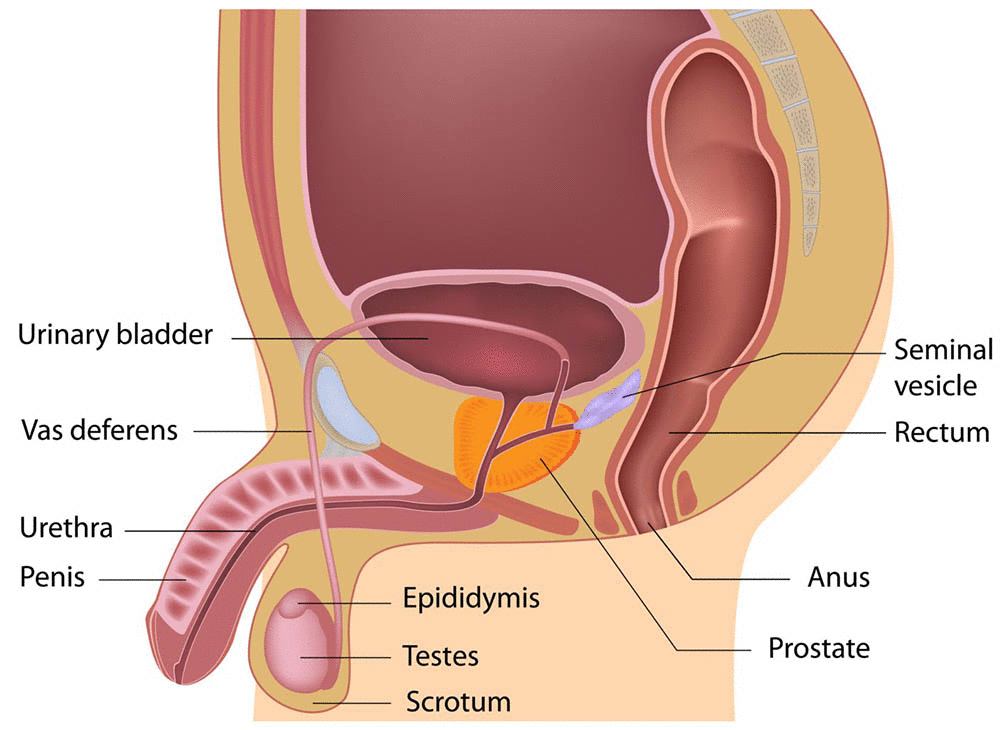
- Sperm produced in testes → enter epididymis
- Mature in epididymis over 2-3 weeks (become motile)
- Stored in vas deferens
- During ejaculation: vas deferens contracts → sperm travels to urethra
- Seminal vesicle and prostate secretions join to form semen
- Ejaculated into the female reproductive tract
- Sperm survive up to 5 days in the female reproductive tract
- Capacitation in the female tract – sperm undergo final preparation for fertilisation
- Sperm penetrates egg at the fallopian tube
Common Disorders of the Male Reproductive System
| Condition | What’s Affected | Impact |
|---|---|---|
| Hypogonadism | Testosterone production | Low libido, fatigue, reduced muscle mass |
| Oligospermia | Low sperm count | Reduced fertility |
| Azoospermia | No sperm in ejaculate | Infertility |
| Varicocele | Testicular veins | Overheats testes; impairs spermatogenesis |
| Erectile dysfunction | Vascular/neurological | Sexual function |
| Benign prostatic hyperplasia (BPH) | Prostate enlargement | Urinary obstruction |
| Prostate cancer | Prostate | Local and systemic effects |
| Cryptorchidism | Undescended testes | Impaired spermatogenesis if untreated |
Testosterone Across the Lifespan
| Life Stage | Testosterone Level | Key Events |
|---|---|---|
| Fetal | High (brief surge) | Genital differentiation |
| Puberty | Rapidly rising | Secondary sexual development |
| Adult (20s-30s) | Peak levels | Optimal reproductive function |
| Middle age (40s+) | Gradual decline (~1%/year) | Andropause symptoms in some |
| Older adult | Lower |
Bottom Line
The male reproductive system is a coordinated network of organs and hormones working together to produce sperm, synthesise testosterone, and enable reproduction. The testes are the central organ – producing both sperm and testosterone under hormonal direction from the hypothalamus and pituitary. Understanding this system provides the foundation for understanding male fertility, hormonal health, and the impact of conditions like hypogonadism, varicocele, and prostate disease.


Leave a Comment